Wounds can be classified due to:
- Manner of their creation
- The nature and extent of the loss of the skin and / or tissue
- The degree of contamination by mechanical and bacterial infection
- Time elapsed since the inception of the wound
- Incidence of associated with wound injuries within the adjacent tissues
Abrasions – the most common form of the wounds are various etiologies abrasions most often associated with little loss of the epidermis. Sometimes, however, there is also the loss of the dermis and subcutaneous tissues.
Bitten wounds/lacerations – usually arise as a result of being bitten or mechanical factors, e.g. while trapping or jamming a limb in “traps” (e.g. manholes, sewer grates, etc.). While attempting to release limbs,often frantically,comes to break the continuity of the skin, muscles and sometimes to tear tissues. The bitten wounds are regarded as highly polluted both mechanically and bacterially.
Puncture wounds – are usually deep penetrating wounds. Some of the puncture wounds have exit holes and are defined as the piercing wounds.
Torn wounds – usually arise as a result of strong mechanical trauma (e.g. road accidents). They are serious deep tissue damage, often detachment of tissues. In the case of this type of injuries occur often also reveal the skeletal elements (e.g. frequently limb joints). These are the most heavily contaminated wounds.
Cuts – common of different etiology. In cuts, there is a break in the skin (or its individual layers). Often cuts are wounds penetrating the deeper layers of tissue (muscle) and sometimes the skeletal elements. In such wounds, it is often to find injuries of the blood vessels, tendons, nerves.
Gunshot wounds – can sometimes be considered a form of puncture wounds. These types of injuries can most often meet at the hunting dogs.
Burns – these types of injuries can occur as a result of thermal burns, chemical, electrical and occasionally due to conducted radiotherapy. There are three degrees of burn wounds:
First degree burns – superficial burns, it is characterized by skin redness and slight swelling. It is characteristic that this degree of burns is accompanied by severe pain.
Second degree burns – penetrates to the dermis layer. On the skin surface forms blisters. This is accompanied by severe pain. Depending on the degree of penetration sometimes are distinguished degrees of burns IIA and IIB.
Third degree burns – penetrates deep into the layers of the subcutaneous tissue including muscles. On the surface of the skin appears black scab or may occur charring of the skin and sometimes muscle. Painfulness is slight but tissue injury is very serious, often irreversible (necrosis).
A separate category are the wounds are decubitus ulcers (bedsores). Arises from a continuous and long term mechanical stress on the soft tissues. This leads to impaired circulation and cellular metabolism. In animals, it occurs most frequently in the vicinity of tumors of the hip, ischial, shoulder blades, the lateral surface of the tibia (lateral condyle), sternum, olecranon and the heel spur. There are various classifications of the degree of development of decubitus ulcers, depending on the observed changes, i.e. from the minor, characterized by a slight reddening area, no fading under the yoke (during the examination), up to major characterized by irreversible changes in the tissues in the form of necrosis of the muscle fascia, and even joint, and bones.
the degree of mechanical and/or bacterial contamination.
- only surgical wounds are clean
- all other to be regarded as polluted with the degree of contamination depending
on the type of wound and the time elapsed since the creation of the wound
A special role in the contamination of wounds plays bacteria (commensal or pathogenic introduced from outside) colonizing the surface of the wound and leading to the formation of the so-called. bacterial biofilm – which is the main obstacle to proper wound healing.
Biofilm is the combined bacterial microcolony (which may consist of various kinds of pathogenic bacteria) forming a multi-layered three-dimensional structure surrounded by extracellular matrix.
- Protects bacteria and other pathogens against “harmful”, for them, external factors as disinfectants, antibiotics and immune cells
- Creates favorable conditions for the continuous proliferation of already settled bacteria and colonization and the development of new bacteria or other pathogens.
- It affects the spread of infection to neighboring healthy tissue.
- It distorts the exchange of gas in the wound and the host cell blocks access to nutrients.
Biofilm is firmly and strongly bonded to the substrate, removing it from the wound surface with normal rinsing (water, soapy water, physiological saline), is not possible. Therefore, you should use appropriate means allowing the efficient removal and prevention of reproduction or formation.
Wound management
Normal wound healing takes place in three interrelated steps/phases:
1. PHASE OF INFLAMMATION
(Exudative preceded by a short-term haemostasis)
2. PHASE OF SKIN-GRANULATION
(Proliferative)
3. PHASE OF MATURING
(Reconstruction)
Infectious microorganisms, debris, the extraneous material (e.g. mechanical impurities), or necrotic tissue are removed from a wound in the inflammatory phase. The wound is covered with a scab, which protects it from adverse external factors including bacteria. The main cellular factors involved in this phase are platelets (haemostasis), neutrophils and macrophages. The inflammatory phase lasts from 1 to 5 days.
In the proliferative phase, inflammatory processes in the wound are inhibited and begins the process of granulation of tissue and filling defects and the process of angiogenesis. The proliferative phase lasts from 5 to 21 days and involves mainly the fibroblasts, lymphocytes, endothelial cells and keratinocytes.
In the final stage takes place maturation, reorganization of the structures of scar tissue formed in the second phase, i.e. the reduction of the resulting scar. This process can last from 3 weeks to up to 2 years. A special role in this process is played by fibroblasts.
However, the healing process very often is disturbed by a number of external and internal factors such as deficiencies in the inflammatory response within the wound, delay in angiogenesis or granulation resulting from e.g. cardiovascular disorders, metabolic diseases, neuropathy or malnutrition. An important factor influencing the external wound healing disorder is heavy contamination of the wound by mechanical or microbiological contaminants. A special role is attributed to the emerging in the wound bacterial biofilm.
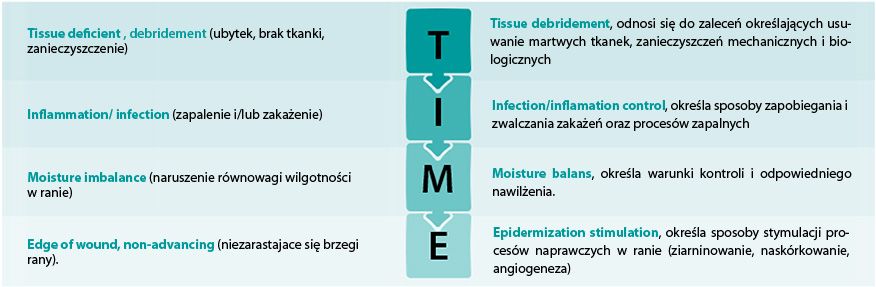
“T I M E” SCHEME
Given the number of problems associated with normal wound healing, and in the light of experience, specialists from the EWMA (European Wound Management Association) proposed in 2003, unified workflow with wounds described as T I M E.
Abbreviation T I M E is an acronym from the first letters of the English names for the various processes and changes (mainly pathological) occurring in wounds and setting out the procedure for the various stages of wound healing.
CHANGES
Specifies the processes and pathological changes occurring in the wounds at different stages
PROCEEDINGS
Each point of the acronym TIME corresponds to EWMA guidelines for proper conduct in the process of wound healing in various stages of:
T I M E is a dynamic scheme subject to constant modifications resulting from both medical knowledge and lessons learned by doctors. For example: the discovery of a specific role played by bacterial biofilm in significant delay in wound healing forced to supplement the scheme with the methods of effective preventing the formation of biofilm in the wound or to control the already formed biofilm. Therefore, were developed methods of combating bacterial biofilm – BBWC (Biofilm-Based Woun Care/Management). One such efficient method (which is a part of the schema in section “T” of T I M E) is lavasepsis i.e.: an irrigation of wounds with special preparations as effective removers and warring bacterial biofilm, as well as cleansing wounds from any other biological and/or mechanical contaminants.